How declining vagal tone, and structural problems at the head-neck junction are reshaping how we understand rheumatoid arthritis — and why upper cervical care belongs in the conversation.
Rheumatoid arthritis is a chronic, progressive autoimmune disease in which the body's own immune system attacks the synovial lining of the joints, producing pain, swelling, stiffness, and over time, joint deformity and disability. Patients are typically managed with disease-modifying anti-rheumatic drugs (DMARDs), biologics, and targeted synthetic agents that suppress the inflammatory response. These medications can be effective, but a meaningful percentage of patients have an inadequate response or cannot tolerate them, leaving them searching for additional answers.
Schedule Your Appointment
Schedule appointmentOver the last two decades, a fundamentally different way of understanding rheumatoid arthritis has emerged from the science of neuroimmunology. Researchers have demonstrated that the immune system is actively regulated by the nervous system — specifically, by the vagus nerve through what is called the cholinergic anti-inflammatory pathway. .
At Neckwise in Sarasota, we focus on a piece of this picture that the conventional rheumatology workup is not designed to evaluate. The vagus nerve emerges from the brainstem, exits the skull through the jugular foramen at the base of the skull, and descends through the upper cervical region on its way to regulating the immune response throughout the body. Structural problems at the head-neck junction can directly disrupt this pathway. For a meaningful number of rheumatoid arthritis patients, the upper cervical spine is not a peripheral detail — it is one of the upstream structural factors that allows chronic immune dysregulation to take hold and persist.
The Vagus Nerve and the Inflammatory Reflex
The cholinergic anti-inflammatory pathway was first described by Kevin Tracey and colleagues in the early 2000s. Through this pathway, the vagus nerve releases acetylcholine, which binds to alpha-7 nicotinic acetylcholine receptors on immune cells and actively suppresses the production of pro-inflammatory cytokines including TNF-alpha, IL-6, and IL-1 beta — the same cytokines that drive joint inflammation in rheumatoid arthritis.
The implications for autoimmune disease became clear when researchers measured vagal activity in patients with rheumatoid arthritis. They found that vagal tone is reduced in RA — and that this reduction can precede the onset of clinical disease. In other words, loss of neural regulation of the immune system appears to be part of how rheumatoid arthritis begins, not just a downstream consequence.
Liboriussen CH, et al. Modulating Heart Rate Variability through Deep Breathing Exercises and Transcutaneous Auricular Vagus Nerve Stimulation: A Study in Healthy Participants and in Patients with Rheumatoid Arthritis or Systemic Lupus Erythematosus. Sensors. 2022. Demonstrated that RA and SLE are associated with impaired autonomic nervous system function and reduced vagal tone.
These findings led to the development of vagus nerve stimulation as a therapy for rheumatoid arthritis. In 2024, the pivotal RESET-RA trial was published, evaluating an implanted vagus nerve stimulator in 242 RA patients who had not responded adequately to biologics or targeted synthetic DMARDs. The results were striking: ACR20 response rates were significantly higher with active stimulation than with sham stimulation at three months, and improved further over twelve months of open-label treatment, reaching 52.8 percent ACR20 response by month twelve. In late 2024, the SetPoint System received FDA approval — the first vagus nerve stimulator approved for an autoimmune disease.
RESET-RA pivotal randomized controlled trial. Nature Medicine, 2025. Vagus nerve-targeted neuroimmune modulation produced significant ACR20 response in patients with rheumatoid arthritis who had inadequate response to biologics. Three quarters of patients achieved symptom relief without additional therapy.
This is no longer theoretical. The principle that activating the vagus nerve modulates the inflammatory response in rheumatoid arthritis is now FDA-approved, peer-reviewed, and supported by phase III pivotal trial data. The relevant clinical question is no longer whether the vagus nerve matters in rheumatoid arthritis. It is how to support its function as effectively as possible.
Why the Upper Cervical Spine Belongs in the Conversation
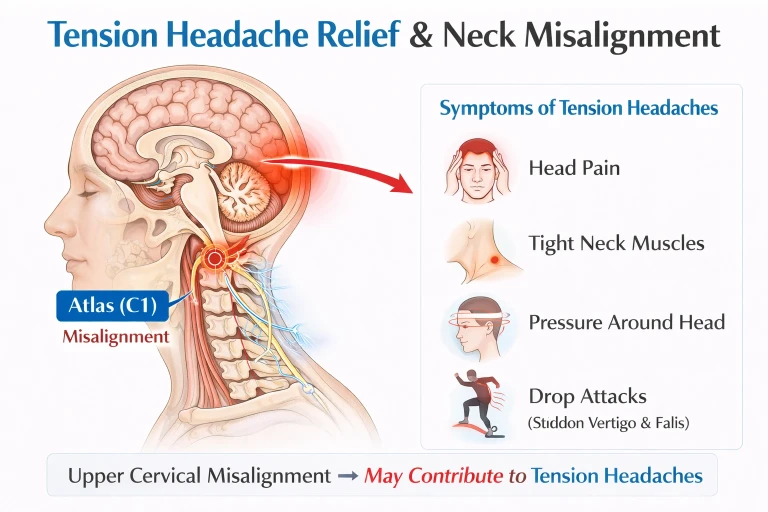
If the vagus nerve plays a central role in regulating the inflammatory response in rheumatoid arthritis, then anything that mechanically irritates the vagus nerve along its path is clinically relevant. This is where the upper cervical spine becomes important.
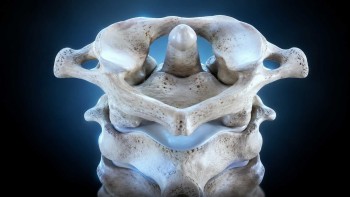
The vagus nerve exits the skull through the jugular foramen, an opening at the base of the skull located immediately adjacent to the atlas vertebra (C1). It then descends through the carotid sheath in the neck on its way to the heart, lungs, gut, and the rest of the body. This path is mechanically vulnerable. The atlas, the topmost vertebra of the spine, has no disc above or below it and depends on a delicate balance of ligaments and small muscles to remain properly aligned. When the atlas shifts even fractions of a millimeter out of its ideal position, the geometry of the entire craniocervical junction changes. The brainstem, where the vagus nerve originates, is subjected to sustained mechanical stress. The jugular foramen narrows. The deep neck muscles compensate with sustained, asymmetric contractions that further compress the soft tissue corridor through which the vagus nerve passes.
The result is a vagus nerve operating under conditions it was not designed for, and a downstream loss of the cholinergic anti-inflammatory signal that the body relies on to regulate immune activation. In a patient already carrying the genetic susceptibility, environmental triggers, and microbiome conditions that contribute to rheumatoid arthritis, this loss of neural regulation can be the missing piece that allows the disease to take hold and become chronic.
The connection between upper cervical structure and autonomic function has been documented in clinical research. A randomized cross-over study published in the Journal of Chiropractic Medicine in 2015 demonstrated that upper cervical spinal manipulation produced measurable improvements in heart rate variability, with shifts toward parasympathetic dominance that were not seen with lower cervical interventions. Heart rate variability is the most widely used non-invasive surrogate measure for vagal tone.
Win NN, et al. Effects of Upper and Lower Cervical Spinal Manipulative Therapy on Blood Pressure and Heart Rate Variability in Volunteers and Patients With Neck Pain: A Randomized Controlled, Cross-Over, Preliminary Study. Journal of Chiropractic Medicine, 2015. Standard deviation of normal-to-normal R-R intervals increased significantly after upper cervical manipulation, indicating enhanced parasympathetic activity.
These findings do not prove that upper cervical care is a treatment for rheumatoid arthritis. They demonstrate that the structural conditions at the upper cervical spine measurably influence the autonomic nervous system that, in turn, regulates the inflammatory response. That mechanistic link is real, documented in peer-reviewed literature, and represents a piece of the rheumatoid arthritis picture that the standard rheumatology workup does not address.
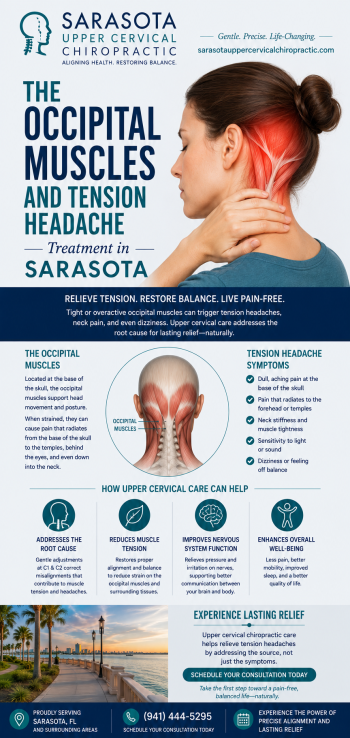
Common Symptoms in Rheumatoid Arthritis Patients We See
Patients with rheumatoid arthritis who come to Neckwise often present with a constellation of symptoms that extends well beyond the joint involvement. The autonomic and neurological pattern is consistent with the underlying loss of vagal tone documented in the research literature. Common symptoms include:
• Joint pain, swelling, and morning stiffness affecting multiple joints, particularly hands, wrists, and feet
• Persistent fatigue that is not relieved by rest
• Brain fog and difficulty concentrating, especially during flares
• Heightened stress reactivity and a sense of being in fight-or-flight
• Heart palpitations or awareness of heart rate changes
• Sleep disturbance and unrefreshing sleep
• Digestive symptoms — bloating, motility changes, food sensitivities
• Neck pain, neck stiffness, or tension at the base of the skull (frequently overlooked in the rheumatology workup)
• Headaches and migraines, particularly during disease flares
• A history of head or neck trauma — sometimes recent, often years or decades old
The presence of cervical and autonomic symptoms alongside the rheumatoid arthritis is one of the strongest signals that the upper cervical spine deserves evaluation.
How Neckwise Evaluates and Corrects
The Neckwise process is built around objectivity. The evaluation begins with a comprehensive consultation and history, with particular attention to the timeline of the rheumatoid arthritis diagnosis, the pattern of associated autonomic symptoms, and prior trauma to the head or neck. Objective testing — including a leg balance test and infrared thermography — determines whether the nervous system is showing measurable signs of upper cervical involvement.
If the screens point toward upper cervical involvement, we move to imaging. Neckwise uses CBCT 3D imaging as a precision tool to visualize the atlas and axis in three dimensions. Unlike a flat X-ray, CBCT produces a true three-dimensional model of the upper cervical region, and the misalignment is quantified in degrees and millimeters across all axes of motion.
The Neckwise correction involves no twisting of the neck, no cracking or popping sound, and no forceful pulling or sudden movement of the head. This matters in general, and it matters even more for patients with rheumatoid arthritis, who often have cervical joint involvement themselves and whose autonomic nervous system is already in a state of heightened sensitivity. The correction is delivered as a controlled, low-force input — gentle enough that many patients are surprised it has happened at all. The intent is to give the body a precise mechanical input that allows it to release the misalignment on its own terms, restoring the structural conditions the brainstem and vagus nerve need to function.
Finding Natural Support for Rheumatoid Arthritis in Sarasota
If you are living with rheumatoid arthritis and searching for natural treatment support in Sarasota, an upper cervical evaluation may be a meaningful piece of your care. The connection between the vagus nerve, the autonomic nervous system, and the immune response in rheumatoid arthritis is no longer theoretical — it is the basis of FDA-approved therapy. The structural conditions at the head-neck junction influence the same nerve that the SetPoint device stimulates electrically. When that structural piece is missing from a patient's evaluation, the picture is incomplete.
Upper cervical care is not a cure for rheumatoid arthritis, and it is not a replacement for rheumatology care, DMARDs, or biologics. It is a structural intervention that addresses one specific, measurable, mechanical factor that is consistently overlooked in conventional management. To learn more or schedule a consultation, contact Neckwise Sarasota.




Leave a comment