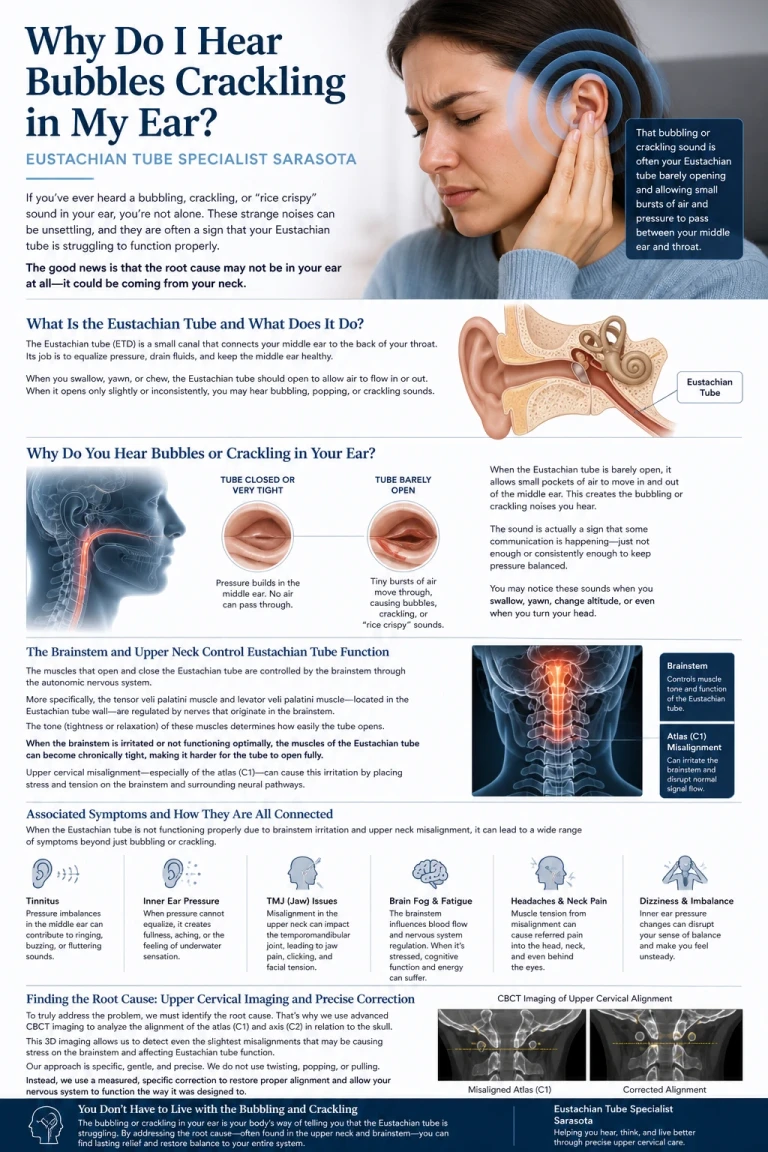
Why You Feel Lightheaded When You Stand Up
If you’ve ever stood up and suddenly felt dizzy, faint, or like your heart started racing, you know how unsettling it can be. For some people, this is not just an occasional moment—it becomes a daily experience. You may notice your vision dimming, your balance shifting, and a sudden awareness of your heartbeat as it speeds up to keep you upright.
Schedule Your Appointment
Schedule appointmentThese symptoms are often grouped under the term dysautonomia, which includes conditions like POTS (Postural Orthostatic Tachycardia Syndrome) and orthostatic intolerance. While these diagnoses describe what is happening, they often don’t fully explain why it’s happening. Many patients are left managing symptoms without ever addressing the root cause.
To understand what may truly be driving these symptoms, we have to look deeper—into the brainstem and its relationship to the upper neck.
Understanding Dysautonomia and the Autonomic Nervous System
Your Body’s Automatic Control System
Dysautonomia refers to dysfunction of the autonomic nervous system, which is responsible for regulating all the automatic functions in your body. This includes heart rate, blood pressure, breathing, digestion, and temperature regulation. These processes happen without conscious effort, constantly adjusting to keep you stable.
At the center of this system is the brainstem. It acts as a command center, monitoring internal conditions and making rapid adjustments as your body changes position or encounters stress. When this system is working properly, you can move from lying down to standing without even thinking about it. When it is not functioning well, that simple transition can trigger a cascade of symptoms.
The Brainstem: The Control Center for Blood Pressure and Heart Rate
How Your Body Adapts to Gravity
When you stand up, gravity immediately pulls blood downward into your legs and abdomen. Without compensation, this would reduce blood flow to your brain and cause you to pass out. To prevent this, the brainstem initiates a rapid response through the autonomic nervous system.
This response includes tightening blood vessels, activating surrounding muscles, adjusting heart rate, and coordinating blood flow so that enough circulation reaches the brain. All of this happens in a matter of seconds and is usually so seamless that you never notice it.
The “Gate” System in Your Veins
How Blood Stays in the Right Place
Inside your veins are one-way valves that act like gates, ensuring that blood flows in the proper direction. These gates are essential when moving against gravity, especially when you stand up. The brainstem controls the timing and coordination of these gates through autonomic signals.
When functioning properly, these valves close efficiently and work with muscular contractions to push blood back up toward the heart and brain. This allows you to remain stable and conscious.
What Happens When the System Is Delayed
If the signals from the brainstem are delayed or disrupted, those gates do not close quickly enough. Blood begins to pool in the lower body instead of staying in circulation where it is needed most.
As blood drains away from the brain, you may feel lightheaded, dizzy, or even close to fainting. Your body responds by increasing your heart rate in an attempt to compensate, which is why many people experience tachycardia alongside these symptoms. The issue is not just the heart racing—it is the system trying to correct a deeper imbalance.
The Missing Link: Upper Neck Misalignment and Brainstem Irritation
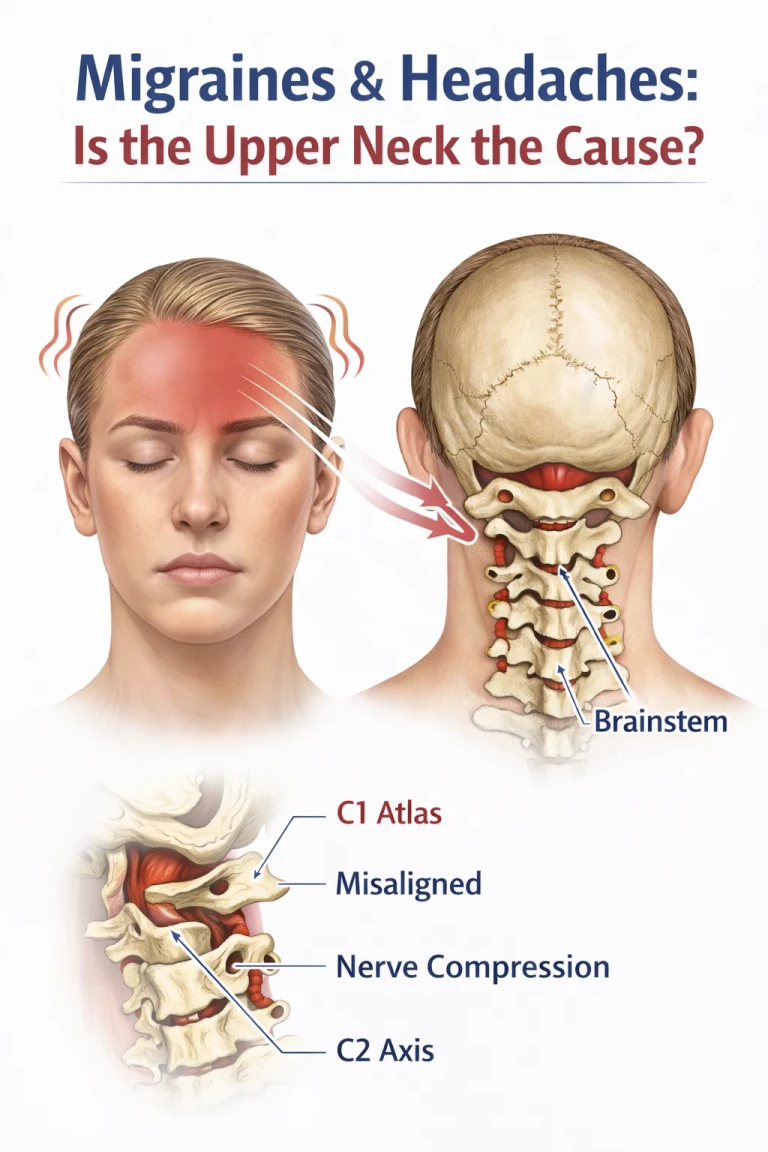
The Role of the Atlas
The atlas, or C1 vertebra, sits at the very top of your spine and supports the skull. It surrounds the brainstem and plays a critical role in protecting and positioning this vital structure. Because of its location, even a slight misalignment can influence how the brainstem functions.
This is not about a dramatic compression or obvious injury. Instead, it involves subtle mechanical stress and altered signaling that can disrupt communication within the nervous system.
How Misalignment Affects Autonomic Function
When the atlas is misaligned, it can create irritation around the brainstem. This interference affects how signals are processed and transmitted. The result is a delay or disruption in the body’s ability to regulate blood pressure, heart rate, and vascular tone.
This is where the connection becomes clear. If the brainstem cannot send timely signals, the venous gates may not close properly. Blood may pool where it shouldn’t, leading to reduced circulation to the brain and triggering symptoms like dizziness and tachycardia.
Why Dysautonomia Symptoms Feel So Widespread
The Brainstem’s Broad Influence
One of the most confusing aspects of dysautonomia is how many different symptoms can occur. Beyond feeling faint when standing, people often experience fatigue, brain fog, anxiety, digestive issues, headaches, and temperature sensitivity.
These symptoms may seem unrelated, but they all trace back to the brainstem. This structure regulates multiple systems at once, so when it is not functioning optimally, the effects can be widespread.
A System in Overdrive
When the autonomic nervous system is dysregulated, the body often becomes reactive rather than adaptive. Instead of making smooth adjustments, it overcompensates. This is why the heart may race excessively, or why symptoms may feel unpredictable and overwhelming.
How Upper Neck Injury Contributes to the Problem
Small Injuries Can Have Big Effects
Many people do not associate their symptoms with a past neck injury, especially if it seemed minor at the time. Events such as car accidents, sports impacts, falls, or even prolonged poor posture can shift the alignment of the upper cervical spine.
These changes may not cause immediate pain, but over time they can affect how the brainstem functions and how the nervous system communicates.
The Delayed Onset of Symptoms
It is common for symptoms to appear gradually. The body often compensates for a period of time, adapting to the misalignment. Eventually, however, the stress on the system becomes too great, and symptoms begin to surface.
This delayed pattern can make it difficult to connect the dots between cause and effect.
Why Traditional Testing Often Falls Short
The Difference Between Structural and Functional Problems
Standard medical imaging is excellent at identifying structural damage, such as fractures or significant abnormalities. However, many cases of dysautonomia involve functional disturbances rather than visible structural issues.
This means that tests may come back normal, even though the system is not working correctly.
Searching for Answers
Because the upper cervical spine is not always evaluated in detail, many patients are left without clear answers. They may be told their symptoms are stress-related or unexplained, which can be frustrating when the symptoms are very real.
The Role of CBCT Imaging in Precision Diagnosis
Seeing the Upper Cervical Spine Clearly
Cone Beam Computed Tomography (CBCT) provides a detailed, three-dimensional view of the upper cervical spine. This allows for precise measurement of the atlas and axis alignment relative to the skull.
Rather than relying on assumptions, this technology provides objective data that guides care.
Why Precision Matters
The upper cervical spine is a highly sensitive area where small misalignments can have significant neurological effects. CBCT imaging allows for accurate analysis and targeted correction, ensuring that care is tailored to each individual.
A Different Approach: Gentle, Precise Correction
No Twisting, Popping, or Pulling
Upper cervical chiropractic care focuses on restoring alignment without aggressive manipulation. The corrections are gentle and highly specific, designed to reduce stress on the brainstem and improve nervous system function.
This approach avoids the forceful techniques that many patients are concerned about.
Restoring Balance in the Nervous System
When the atlas is properly aligned, communication between the brainstem and the body begins to improve. Signals regulating blood pressure, heart rate, and vascular tone become more efficient.
As a result, the timing of the venous gate system improves, helping maintain proper blood flow to the brain during positional changes.
What Patients Often Experience
Gradual Improvements in Symptoms
As the nervous system begins to regulate more effectively, patients often notice a reduction in dizziness and fewer episodes of rapid heart rate. Energy levels may improve, and mental clarity often returns.
These changes reflect the body’s ability to regain stability rather than constantly compensating.
A Return to Normal Function
Over time, many patients describe a sense of normalcy returning. The fear of standing up and feeling faint begins to fade, and daily activities become more manageable.
Dysautonomia Specialist in Sarasota: A Root Cause Perspective
If you are experiencing symptoms like feeling faint upon standing or dealing with tachycardia, it is important to recognize that your body is responding to an underlying issue. The connection between the upper neck, brainstem, and autonomic nervous system is often overlooked but can be critical.
By addressing this relationship, it is possible to move beyond symptom management and toward true correction.
Final Thoughts: Your Body Is Trying to Protect You
The symptoms you are experiencing are not random failures—they are your body’s attempt to adapt. The racing heart, the dizziness, and the fatigue are all compensatory responses to a system that is struggling to regulate itself.
When the brainstem is functioning clearly and the nervous system is communicating effectively, those compensations are no longer necessary.
Understanding the role of the upper cervical spine may provide the missing piece. By restoring alignment and reducing interference, the body can begin to function the way it was designed to—bringing stability, clarity, and lasting relief.


Leave a comment