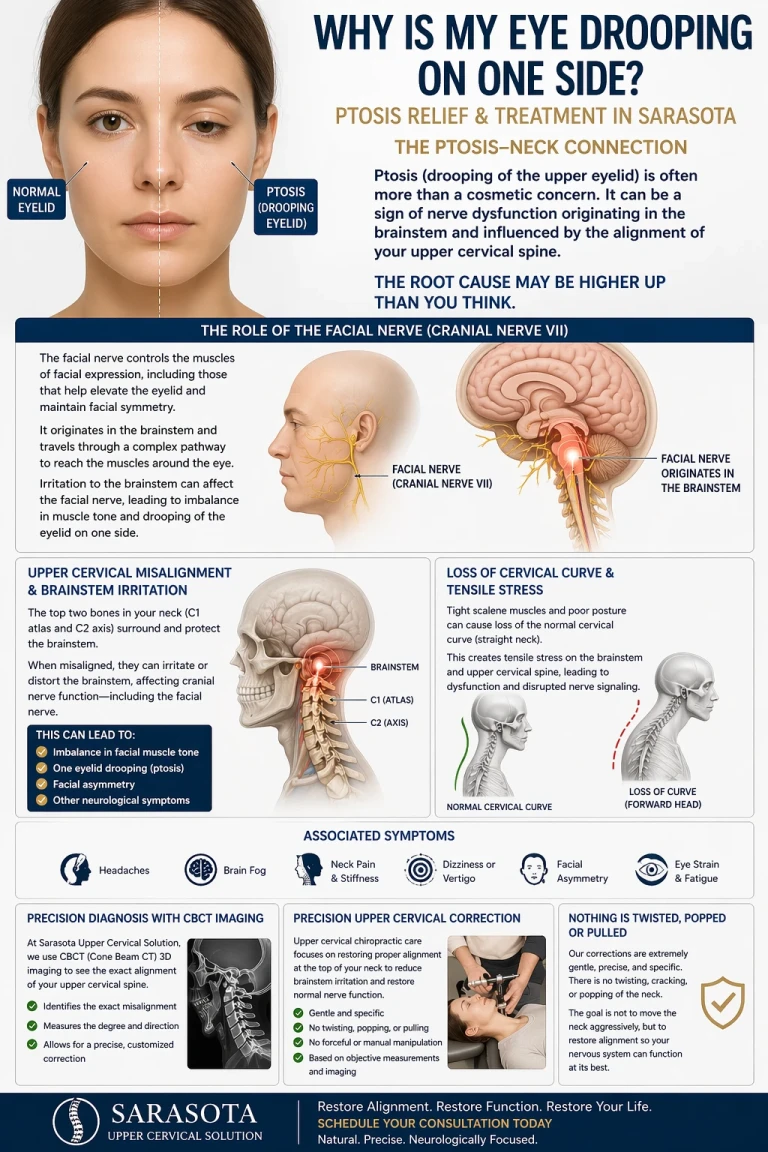
Waking up and noticing that one side of your face isn’t moving properly can be alarming. You may see:
One side of your mouth drooping
Difficulty closing one eye
An uneven smile
Facial weakness or numbness
Schedule Your Appointment
Schedule appointment
In many cases, this presentation is diagnosed as Bell’s palsy—a condition involving dysfunction of the facial nerve.
But here’s the critical question most people are never asked:
Why did the facial nerve become dysfunctional in the first place?
To truly understand Bell’s palsy, we need to look deeper—beyond the face—and into the brainstem and upper cervical spine, where these nerves originate and are controlled.
What Is Bell’s Palsy?
Bell’s palsy is a condition characterized by:
Sudden weakness or paralysis of the muscles on one side of the face
Dysfunction of the facial nerve (cranial nerve VII)
This nerve controls:
Facial expression (smiling, blinking, frowning)
Tear production
Saliva production
Taste (front two-thirds of the tongue)
When the facial nerve is irritated, inflamed, or not functioning properly:
The muscles it controls lose tone
One side of the face becomes weak or droops
The Cranial Nerves Involved in Bell’s Palsy
While Bell’s palsy primarily affects the facial nerve (CN VII), several cranial nerves work together to support facial function and sensation:
1. Facial Nerve (Cranial Nerve VII)
Controls facial muscles
Responsible for symmetry of the face
Affects blinking, smiling, and expressions
2. Trigeminal Nerve (Cranial Nerve V)
Provides sensation to the face
Helps coordinate chewing
3. Glossopharyngeal Nerve (Cranial Nerve IX)
Involved in swallowing
Contributes to throat sensation
4. Vagus Nerve (Cranial Nerve X)
Controls autonomic functions
Plays a role in voice and swallowing
5. Hypoglossal Nerve (Cranial Nerve XII)
Controls tongue movement
All of these nerves originate from or are closely associated with the brainstem
This is key.
Because if something disrupts brainstem function, it can affect multiple cranial nerves—not just one.
The Brainstem: The Control Center Behind Facial Function
The brainstem sits at the base of your skull and is responsible for:
Coordinating cranial nerve activity
Regulating muscle tone
Maintaining symmetry and balance in the body
The facial nerve specifically exits the brainstem at the level of the pons, then travels through the skull to innervate the muscles of the face.
When the brainstem is functioning normally:
Nerve signals are clear and balanced
Facial muscles work symmetrically
But when the brainstem becomes irritated or stressed:
Nerve signaling can become distorted
How Upper Cervical Misalignment Can Be a Root Cause
The top two bones in your neck—C1 (atlas) and C2 (axis)—surround and protect the brainstem.
This area is known as the craniocervical junction, and it is one of the most neurologically important regions in the body.
When there is an upper cervical misalignment, it can:
Irritate or compress the brainstem
Disrupt cranial nerve signaling
Alter muscle tone and coordination
What Does This Lead To?
Weakness in facial muscles
Loss of symmetry
Drooping on one side of the face
Bell’s palsy may be the result of brainstem irritation—not just a random nerve issue
The Chain Reaction
Here’s how this process can unfold:
Upper Cervical Misalignment → Brainstem Irritation → Facial Nerve Dysfunction → Muscle Weakness → Facial Drooping (Bell’s Palsy)
This perspective shifts the focus from:
“What’s wrong with my face?”
to
“What’s affecting the nerve controlling my face?”
Common Symptoms of Bell’s Palsy
In addition to facial drooping, Bell’s palsy may include:
Inability to fully close one eye
Uneven smile or facial expression
Drooping of the mouth
Excessive tearing or dry eye
Loss of taste
Sensitivity to sound
Difficulty speaking clearly
Because multiple cranial nerves are involved, you may also experience:
Neck pain or tightness
Headaches
Dizziness or vertigo
Brain fog
Why Conventional Approaches May Miss the Root Cause
Many conventional treatments focus on:
Reducing inflammation
Managing symptoms
Waiting for spontaneous recovery
While some people do improve over time, this approach doesn’t always address:
Why the nerve became dysfunctional in the first place
If the brainstem is under stress due to upper cervical misalignment, the underlying issue may persist.
The Upper Cervical Chiropractic Approach
Upper cervical care focuses on one primary objective:
Restoring proper alignment at the top of the neck to reduce brainstem irritation
This approach is:
Highly specific
Neurologically focused
Based on objective measurements
Adjustments are only performed when testing indicates they are necessary.
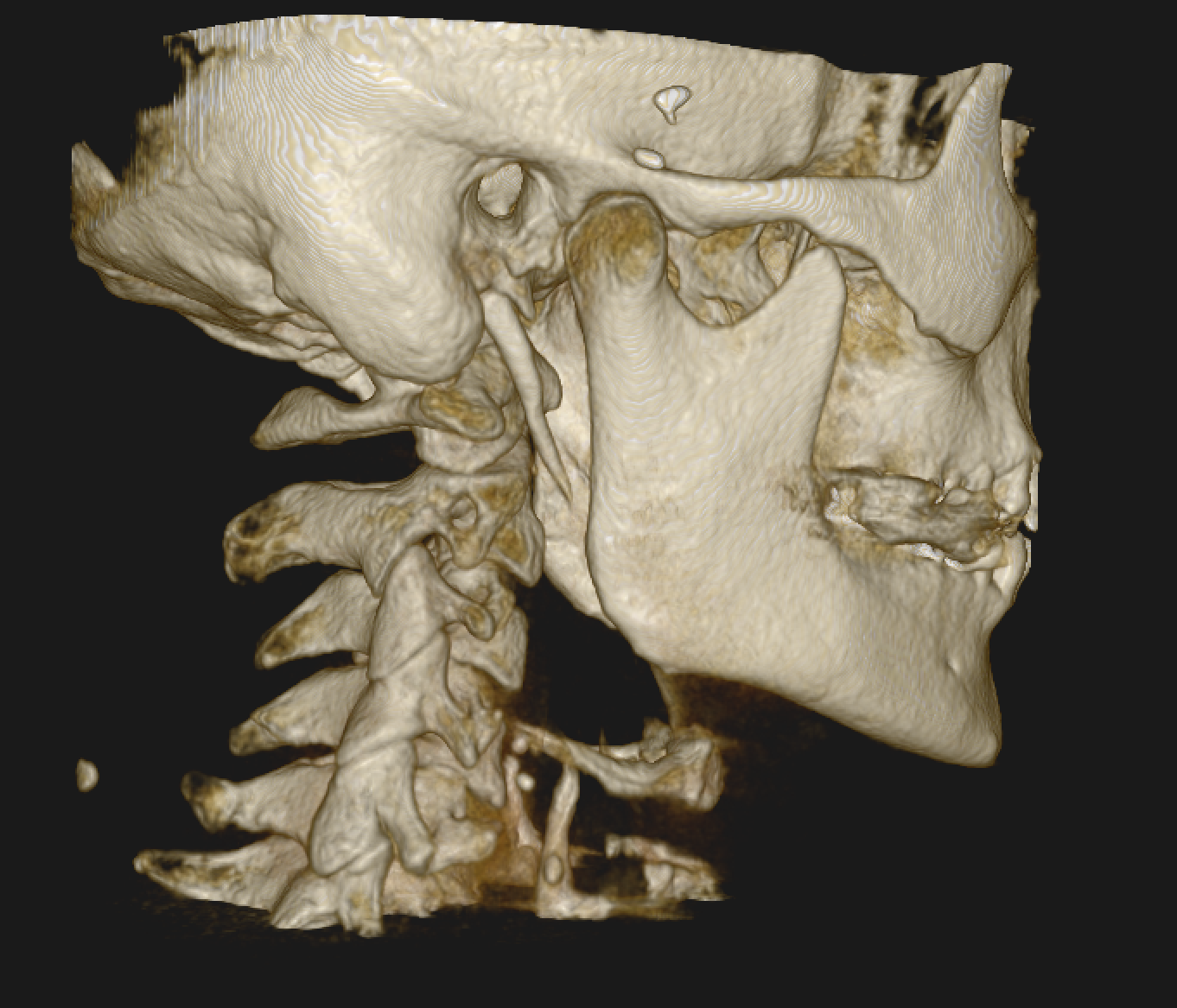
Precision Matters: CBCT Imaging
To determine exactly what’s happening, CBCT (Cone Beam CT) imaging is used.
This advanced imaging provides:
A 3D view of the upper cervical spine
Precise measurement of misalignment
Exact direction and degree of the problem
No guessing. No generalized adjustments.
Every correction is:
Customized
Precise
Based on your unique anatomy
No Twisting, Popping, or Pulling
Upper cervical adjustments are very different from traditional chiropractic techniques.
They are:
Gentle
Specific
Controlled
There is:
No twisting of the neck
No cracking or popping
No forceful manipulation
The goal is not to aggressively move the spine…
👉 It’s to restore alignment so the nervous system can function properly

Leave a comment