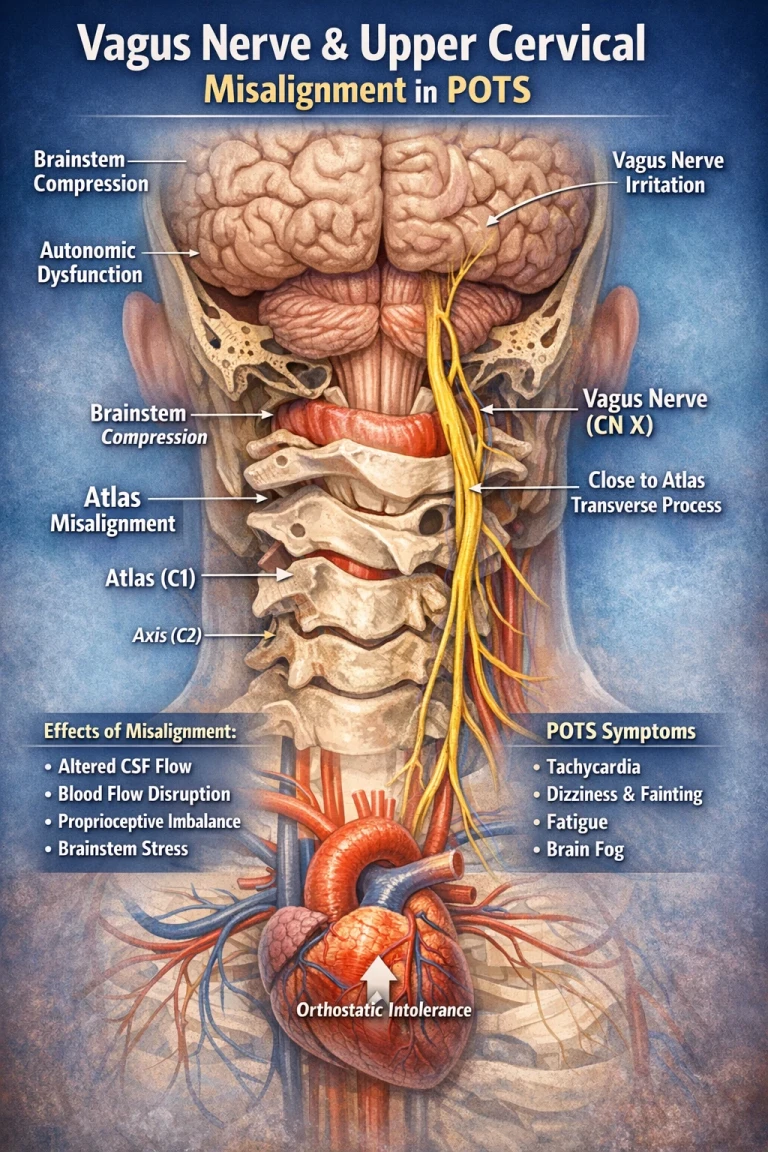
Postural Orthostatic Tachycardia Syndrome (POTS) and broader forms of dysautonomia are increasingly recognized conditions that can dramatically impact quality of life. Patients often report feeling dismissed, misunderstood, or stuck in a cycle of symptom management rather than true resolution. While many approaches focus on medications or lifestyle changes, there is a growing recognition of the role that the nervous system, particularly the brainstem and vagus nerve, plays in regulating these conditions.
At the center of this conversation lies a critical anatomical region: the upper cervical spine, specifically the atlas (C1) and axis (C2). This area is not only structurally unique, but neurologically vital. Subtle misalignments here can create a cascade of dysfunction that affects the autonomic nervous system, and ultimately contributes to symptoms seen in POTS and dysautonomia.
Schedule Your Appointment
Schedule appointmentSchedule a FREE consultation by clicking this here.
Understanding the Vagus Nerve and Autonomic Balance
The vagus nerve is the primary parasympathetic nerve of the body. It originates in the brainstem and travels down through the neck into the chest and abdomen, influencing:
Heart rate
Blood pressure
Digestion
Respiratory rate
Immune and inflammatory responses
In a healthy system, the vagus nerve helps maintain balance between the sympathetic (“fight or flight”) and parasympathetic (“rest and digest”) systems. However, when vagal tone is disrupted or impaired, the body can become stuck in a state of sympathetic dominance—leading to many of the hallmark symptoms of POTS.
This is where structure becomes critical.
The Brainstem: The Control Center at Risk
The brainstem sits at the base of the skull, directly above the atlas (C1). This region houses the nuclei that regulate autonomic function, including those that give rise to the vagus nerve.
When there is trauma—such as a concussion, whiplash injury, or repetitive postural stress—the alignment of the atlas and axis can shift. Even slight misalignments can create:
Mechanical irritation to the brainstem
Altered cerebrospinal fluid (CSF) flow
Disruption in blood flow in and out of the cranial vault
Abnormal signaling through autonomic pathways
Because the brainstem is responsible for regulating heart rate, blood vessel tone, and blood pressure, even minor interference can lead to widespread dysfunction.
Book a FREE consultation by booking here.
Atlas and Axis Misalignment: A Silent Driver of Dysautonomia
The atlas (C1) is uniquely designed, it has no disc above or below it and supports the weight of the skull. The axis (C2) allows for rotation of the head. Together, they form the most neurologically dense and mechanically sensitive region of the spine.
When misalignment occurs in this region, several things can happen:
The proximity of C1 to the brainstem means that even small positional changes can affect neural communication.
2. Altered Proprioceptive Input
The upper cervical spine contains a high density of mechanoreceptors that provide the brain with information about head position and movement. When joints are misaligned, this input becomes distorted—leading to dysregulation of autonomic responses.
3. Dysafferentation
This refers to abnormal sensory input into the central nervous system. When the brain receives conflicting information from the upper neck, it can misregulate heart rate, blood pressure, and vascular tone.
The Cervical Curve and Brainstem Stress
A healthy cervical spine has a natural lordotic (backward C-shaped) curve. This curve is not just structural, it plays a crucial role in distributing mechanical stress.
When the cervical spine straightens, often due to poor posture, trauma, or chronic muscle tension, it places increased strain on the brainstem and spinal cord.
This can lead to:
Increased tension on neural tissue
Reduced shock absorption
Altered biomechanics of the upper cervical joints
Increased likelihood of vagus nerve irritation
Over time, this structural stress can contribute to autonomic dysfunction, especially in individuals already predisposed to POTS.
The Vagus Nerve and the Atlas Transverse Process
One of the most overlooked anatomical relationships in dysautonomia is the close proximity of the vagus nerve to the transverse process of the atlas (C1).
As the vagus nerve exits the skull, it travels just anterior to this bony structure. When the atlas is misaligned, it can:
Alter the spatial relationship between the bone and nerve
Create mechanical irritation or tension
Influence vagal signaling
Additionally, changes in posture, such as forward head carriage, can further compress or tension this region, compounding the issue.
If the vagus nerve is not functioning properly, the body may struggle to regulate heart rate and blood pressure when transitioning from lying down to standing—one of the defining features of POTS.
Common Symptoms of POTS and Dysautonomia
Patients with POTS and dysautonomia can present with a wide range of symptoms, often affecting multiple systems. These include:
Cardiovascular Symptoms
Rapid heart rate upon standing (tachycardia)
Heart palpitations
Lightheadedness or dizziness
Fainting or near-fainting (syncope)
Blood pressure fluctuations
Neurological Symptoms
Brain fog
Difficulty concentrating
Headaches or migraines
Dizziness or vertigo
Sensitivity to light and sound
Autonomic and Systemic Symptoms
Chronic fatigue
Exercise intolerance
Temperature regulation issues
Excessive sweating or inability to sweat
Cold hands and feet
Gastrointestinal Symptoms
Nausea
Bloating
Constipation or diarrhea
Delayed gastric emptying
Other Common Complaints
Anxiety or panic-like symptoms
Shortness of breath
Chest discomfort
Sleep disturbances
Because these symptoms overlap with many other conditions, patients are often misdiagnosed or told that their symptoms are “all in their head.” In reality, there is often a structural and neurological component that has been overlooked.
Evaluating the Upper Cervical Spine in POTS Patients
Upper cervical chiropractors take a different approach to evaluating patients with dysautonomia. Rather than focusing solely on symptoms, they assess the structural integrity of the upper neck and its impact on the nervous system.
1. Leg Balance Assessment
This test evaluates functional leg length differences, which can indicate imbalances in muscle tone and postural control. These imbalances are often driven by altered neurological input from the upper cervical spine.
When a patient lies down, subtle differences in leg length can reflect how the brain is interpreting body position. Changes in leg balance before and after a correction can provide insight into neurological improvement.
2. Infrared Thermography
Infrared thermography measures heat patterns along the spine. Because the autonomic nervous system regulates blood flow to the skin, asymmetrical temperature patterns can indicate areas of dysfunction.
Consistent thermal patterns often correlate with upper cervical misalignments. This allows practitioners to determine:
When a patient is out of alignment
When a correction is needed
When the body is maintaining stability
This objective data helps guide care and avoid unnecessary adjustments.
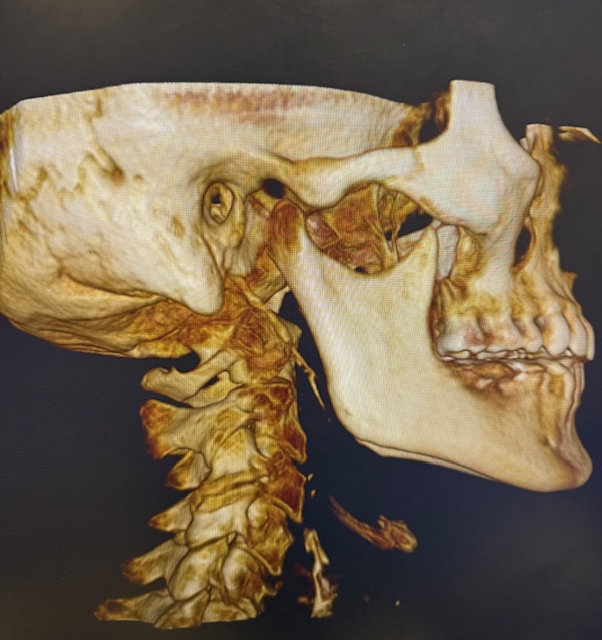
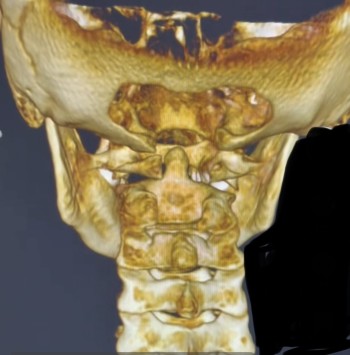
Precision Matters: The Role of 3D CBCT Imaging
One of the defining features of modern upper cervical care is the use of Cone Beam Computed Tomography (CBCT).
Unlike traditional X-rays, CBCT provides a three-dimensional view of the atlas and axis, allowing for:
Precise measurement of misalignment
Visualization of asymmetry in all three planes
Individualized analysis for each patient
No two misalignments are the same. This level of detail ensures that corrections are tailored specifically to the patient’s anatomy.
Gentle, Precise Corrections ,No Twisting or Popping
A major misconception about chiropractic care is that it involves forceful twisting or cracking of the neck. Upper cervical care is fundamentally different.
Corrections are:
Gentle
Specific
Based on precise measurements from CBCT imaging
Delivered without twisting, popping, or pulling
The goal is not to repeatedly adjust the spine, but to make a precise correction and allow the body to stabilize and heal.
When alignment is restored, many patients experience improvements in:
Heart rate regulation
Blood pressure stability
Energy levels
Cognitive clarity
Overall autonomic balance
Connecting the Dots: Structure and Function
POTS and dysautonomia are complex conditions, but they are not random. The body is responding to underlying dysfunction—often rooted in the nervous system.
When the upper cervical spine is misaligned, it can:
Irritate the brainstem
Disrupt vagus nerve function
Alter proprioceptive input
Impair blood and CSF flow
Create a cascade of autonomic imbalance
By addressing the structural component, specifically the alignment of the atlas and axis—upper cervical care aims to remove interference and allow the nervous system to function as designed.
A Different Approach for Sarasota Patients
For patients in Sarasota dealing with POTS and dysautonomia, this approach offers a different perspective—one that looks beyond symptom management and focuses on restoring proper neurological function.
Rather than masking symptoms, the goal is to:
Identify the root structural cause
Make precise, individualized corrections
Support the body’s natural ability to regulate itself
Final Thoughts
The vagus nerve plays a central role in autonomic regulation, but it does not function in isolation. Its health is deeply connected to the structure and integrity of the upper cervical spine and the brainstem.
In cases of POTS and dysautonomia, overlooking this relationship may mean missing a key piece of the puzzle.
By understanding how atlas and axis misalignments influence the nervous system—and by using advanced imaging and precise correction techniques—patients have an opportunity to address the root cause of their symptoms and move toward lasting improvement.
If you or someone you know is struggling with POTS, dysautonomia, or unexplained neurological symptoms, it may be time to consider whether the upper cervical spine is playing a role.





Leave a comment